The human brain rests in cupped hands as easily as a cantaloupe. It is softer and spongier to the touch, of course, and its surface is more deeply ridged and wrinkled than the melon's skin. Since the time of Hippocrates, physicians and scientists have contemplated the brain and wondered not only how it gives rise to everything we feel, know, accomplish, and create, but also how all this can be stolen by injury or disease.
It wasn't until the invention of the microscope, in the seventeenth century, that scientists were able to examine nerves in any detail. By the early nineteenth century, pioneering physiologists had traced those fibers to the brain and made some observations that hold true today. They figured out, for example, that pulling back from a hot stove was a reflex, not a conscious action. They also learned that different regions of the brain govern distinct functions, knowledge that enabled doctors to examine a head injury and predictat least in a crude waywhether it was more likely to leave the patient crippled or sightless.
In 2002, these insights seem primitive, dwarfed by the twentieth-century revolution in neuroscience and its clinical partner, neurology. Modern science has reduced the throwing of a ballor a tantrumto millions of details that can be described in the precise language of biochemistry, genetics, and molecular biology. Although medicine has benefited from knowing millions of individual facts about the brain, the dean of Harvard Medical School (HMS), Joseph B. Martin, a neuroscientist himself, says that the next step is "putting Humpty Dumpty back together." He is confident that assembling a more holistic, integrated model of brain function will lead to better, safer treatments for stroke, memory loss, Parkinson's disease, and other major disorders.
 |
| Carla J. Shatz, chair of the neurobiology department at Harvard Medical School, maps neural transmissions in her laboratory. |
| Photograph by Tracy Powell |
As neuroscience shifts gears, something else remarkable is happening at HMS: the latex-gloved hands that hoist the brain like a melon or, more accurately, feed a few of its cells into a high-powered analyzer, are increasingly likely to be the hands of a woman. Carla J. Shatz '69, Jf '76, Ph.D.'76, chairs the department of neurobiology and is the first and only woman to head a basic-science research department at the medical school. Anne Buckingham Young, M.D.-Ph.D., is chief of the neurology service at Massachusetts General Hospital (MGH); she is not only the sole female department head, but also the only female neurology chief at any academic medical center in the United States. As prominent as Shatz and Young are in the world of brain research, they are not alone at the medical school. Around them are numerous researchers who are not only young and gifted, but female as well. Investigators Li-Huei Tsai and Junying Yuan, Ph.D. '89, who have each made important discoveries about disease and injury in the brain, are representatives of neuroscience's next wave.
"Cells that fire together, wire together": Mapping Brain Function
Carla Shatz and the department she now chairs grew up together. In the summer of 1966, after her first year at Radcliffe, HMS elevated neurobiology from mere laboratory to full-fledged department. People were turning on, tuning in, and dropping out, and by the standards of the time, Shatz was probably a bit of a grind. Her father, a scientist, and her mother, an artist, had encouraged her to excel in West Hartford's demanding public-school science curriculum. At Radcliffe, she was one of only two women concentrating in chemistry. By the start of her senior year, however, she realized that it wasn't her true calling.
"I was really interested in how we see," Shatz recalls. She had been captivated by Nobel laureate George Wald's course on the chemistry of vision and Rudolf Arnheim's class on visual perception, which emphasized that science could contribute to debates about art. But even more important was her mother's influence. "Her painting got me interested in vision from the artistic side, and in some subliminal way guided my decision to work on the visual system."
Shatz's undergraduate adviser suggested that she seek a tutorial with David H. Hubel, a physiologist at the medical school (and now research professor of neurobiology) who studied vision. A tutorial would allow her to graduate with honors and still enable her to begin the transition from chemistry to biology. Shatz telephoned "out of the blue, and at first I was skeptical," Hubel recalls. "But I said, "What the heck.'" Every week she handed him an essay about a scientific article he had given her to read, and every week, he adds, "I covered them with red ink."
A Marshall Scholarship took Shatz to University College London, where she earned a master's degree in physiology. Meanwhile, back in Boston, women were registering gains on campus. In 1969, the year that Shatz graduated, anatomist Elizabeth Hay (now Pfeiffer professor of embryology) was named the first female full professor in a basic research department at HMS.
When Shatz returned from London, she immediately petitioned Hubel and his research partner, Torsten Weisel, to accept her as a Ph.D. student, even though they rarely took anyone more lowly than a postdoctoral fellow. "I told her she could do it, but she would have to work like hell," Hubel says with a chuckle.
Shatz had apprenticed herself to investigators who thumbed their noses at the notion that the human brain could not comprehend its own complexity. "Nonsense. The brain can be studied just as the kidney can," was Hubel's retort. Employing the cutting-edge technology of their time, Hubel and Weisel used tiny electrodes to stimulate a single nerve cell and then recorded the chain of electrical messages it sent to other cells. Thousands of individual measurements were required to construct a map showing how input from the eyes journeys to the back of the brain, where the visual cortex transforms these signals into what we see. They also discovered that these pathways are established during a critical period early in life, and that blocking signals during that time will result in permanent visual impairment. These findings earned them the 1981 Nobel Prize in physiology.
Shatz's own research built on theirs. En route to the visual cortex, signals from the eye are channeled through circuits in the lateral geniculate nucleus (LGN), a part of the thalamus. Shatz was the first to show that before birth, the fetal retina sends messages that begin sorting "a jumble of wires" in the LGN into layers. Once a human baby or animal is born, light striking the retina triggers electrical impulses that bombard the LGN, refining its structure into highly organized layers that efficiently transmit information to the visual cortex. Brain cells that don't see any action are "pruned" as a part of normal development. Although Shatz has used the visual system to demonstrate this "use it or lose it" principle, the same process holds for other forms of learning and memory. "Cells that fire together, wire together," she says.
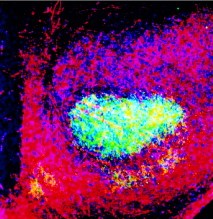 |
| An image of the lateral geniculate nucleus showing the millions of connections made by retinal ganglion cells from the left eye (red outer ring) and the right (turquoise center). |
| Courtesy of Carla J. Shatz |
Now the one-at-a-time approach is being supplanted by all-at-once technologies that make it possible to study thousands of cells, genes, or proteins. "Even the simplest action involves more than one nerve cell at a time, so the goal is to study the functioning of many, many cells simultaneouslyand we can't do that without computers," Shatz says. For example, her lab uses a high-tech imaging system that takes tiny blips of electricity emitted by whole groups of neurons and converts them into pictures so that scientists can watch as thousands of brain cells pass along a message. Viewed on a monitor, this looks like "the wave" rippling through the bleachers at Fenway Park. Not surprisingly, in a modern biology lab the computers outnumber the people.
In 1998, a massive gene screen led to one of the most remarkable findings yet to emerge from the Shatz lab. Postdoctoral fellows Gene Huh and Lisa Boulanger set out to identify every gene activated in nerve cells during normal development. Mostly they found genes they already knew well, but one was as out of place as a peach pit in a melon: the gene encoding a major immune-system molecule, class I MHC, was turned on while normal neural connections were forming. Class I MHC proteins are common elsewhere in the body, where they bind tiny snippets of invading viruses and bacteria and display them on the surface of infected cells, causing defensive T cells to swoop down and destroy theman essential function of a healthy immune system. "Nerve cells weren't even supposed to have these molecules," Shatz says.
When the researchers examined mice that lacked the class I MHC gene, they found abnormalities not only in the LGN, the brain region Shatz knows best, but also in the hippocampus, which is essential for memory. In mice with normal class I MHC, the gene kicks in during early development, shuts down during the animal's prime, then switches on again in later life. Late-life expression was prominent in the hippocampus and other regions involved in learning and memory. Shatz speculates that in neurodegenerative diseases such as Parkinson's or Alzheimer's, class I MHC may mistakenly signal the immune system to attack brain cells, much as it mistakenly destroys the joints in rheumatoid arthritis.
When scientists are chasing a new finding like this, research is "like reading a good novel, where you can hardly wait to find out what happens on the next page," Shatz says. Her own quest to understand the brain has taken her from coast to coast and back again. After finishing her training at HMS, she spent 14 years at Stanford's School of Medicine. There she gained a national reputation and in 1985 became one of the school's few tenured women. It was a tumultuous time for women at Stanford: a study of faculty salaries by gender was scrapped when there were too few women to constitute a statistically valid sample, and in 1991 neurosurgeon Frances K. Conley caused a huge flap by resigning over the imminent promotion of a male colleague that she thought could be explained only by ingrained sexism at the medical school. (She later returned, but also wrote a scathing memoir about her experiences, Walking Out on the Boys; it appeared in 1998.)
Shatz herself was upset because the medical school, which routinely found suitable posts for the wives of male faculty members, seemed unable to do the same for her husband. The University of California-Berkeley made attractive offers to them both, and in 1992 Shatz voted with her feet and moved across San Francisco Bay. At Berkeley, she and her laboratory earned both luster and financial support when she was selected as a Howard Hughes Medical Institute investigator. Although she says she learned a great deal from being part of Berkeley's distinguished biology department, she also felt isolated from neuroscientists, who are concentrated mostly at medical schools throughout the world.
She was thrilled when Joseph Martin invited her to return to Harvard as chair of neurobiology. By now she was divorced and free to move, and she knew that returning to HMS would put her where the action was in her own field. There was another reason as well, which she describes as "a woman's thing: I felt personally very grateful to Harvard. I wanted to give back, if I could, some of the things I had gotten." She pauses, and then a mischievous glint comes into her eyes. "Besides, if I turned down the opportunity, it wasn't clear that the next person on the list was going to be a woman." Martin says that Shatz was an obvious choice to lead the department: "Carla is one of the single most distinguished people in neurobiology, period. Being a woman is only incidental." He calls her work "a series of landmark studies," adding that the discovery of class I MHC molecules in the brain has "extraordinary importance."
Today, Shatz leads a department with 200 people, including 14 full professors, that is awarded about $7 million in grants each year. Her own laboratory has a staff of 18, including six postdocs in physiology and molecular biology. She was instrumental in the creation of the Harvard Center for Neurodegeneration and Repair (CNR) and leads one of its core activitiesthe HMS center for brain imaging. (The CNR combines the talents of researchers on the HMS Quad with those of physicians and scientists at six of Harvard's hospital and research affiliates. Launched in early 2001 with a $37.5-million, private, seed-money grant, the center is establishing five core components that will make specialized technologies and training available to all Harvard brain researchers. In addition to Shatz's imaging center, other cores will provide sophisticated information management, molecular diagnosis of neurodegenerative diseases, automated chemical screening, and translational researchan essential service for helping scientists move basic discoveries into product development. More information is available at www.hcnr.med.harvard.edu/.)
As aging baby boomers fall prey to strokes, Alzheimer's, Parkinson's, and similar conditions, they will expect help from elite research institutions like Harvardand not just from its medical school. Shatz, who like other top neuroscientists believes that major medical advances are likely to arise from fortuitous observations in basic-science laboratories, is working hard to improve collaboration between HMS and the Faculty of Arts and Sciences and is playing a role in an integrative neuroscience initiative at FAS. Adding momentum is the return to Harvard, as provost, of Steven E. Hyman, M.D. '80, a distinguished psychiatrist and molecular biologist himself. Hyman's experience as head of the National Institute of Mental Health gives him a strong appreciation for the connection between basic science and patient care. With that perspective, the University may be in a favorable position to draw together its strengths in both pure and applied neuroscientific research. Thus the path Shatz pioneeredfrom a fascination with painting and sight to the exploration of the brain's inner workingsmay become increasingly popular among scientifically inclined students.
Migrating Neurons: Brain Structure and the Lattice of Alzheimer's Disease
Recent events in the lab of Li-Huei Tsai illustrate the importance of chance, at least for an investigator prepared to make the most of it. Tsai was a postdoc in cancer research when a fortuitous discovery led her to switch to neuroscience. The rest is history: pharmaceutical companies are using her findings to develop new drugs for Alzheimer's disease (AD), and Tsai, now associate professor of pathology, has been named a Howard Hughes Medical Institute investigator. HMS dean Martin calls her "one of the most productive young women in the country."
 |
| Li-Huei Tsai's childhood encounter with her grandmother's dementia foreshadowed her research on Alzheimer's disease. |
| Photograph by Tracy Powell |
Tsai's first, most unforgettable, encounter with Alzheimer's occurred even before she started school. Her parents worked in urban Taipei, and during the week she lived with her grandmother in a village outside the city. Every day, the little girl and the old woman walked to a bustling outdoor vegetable market. One rainy day, as they started for home, her grandmother froze and asked with alarm, "Where are we?"
"That incident is such a clear picture in my mind," Tsai says now. "She looked so confused and emotional." The two waited out the shower in a vendor's shed, and when the rain passed, "I led her home." This event troubled Tsai greatly, and her mother later explained that her beloved grandmother was developing dementia.
Tsai did not immediately resolve to try to cure AD. She enrolled in veterinary college, imagining that this was the path to a pleasant, bucolic life. Once she got a taste of laboratory research, however, her goals changed radically. Soon she was fired up about graduate study in the United States, and in 1984 entered a master's program in molecular biology at the University of Wisconsin. From there she went to the University of Texas Southwestern Medical Center, in Dallas, and just as she was about to finish her Ph.D., she met her future mentor at a scientific meeting. She heard Edward Harlow talk about his work on genes that suppress cancer and knew immediately that it was for her.
She applied for a postdoc in Harlow's lab at Cold Spring Harbor Laboratory, was accepted, and arrived on Long Island only to be told that Harlow had taken a position at HMS, where, as professor of biological chemistry and molecular pharmacology, he chairs the department of the same name. His lab picked up and moved to Boston within months, making Tsai think it was just as well that her husband, a software engineer, had kept his job in Dallas. (They were later reunited in Boston.)
Her four years in the Harlow lab were unforgettable. "When I worked with Ed, he was a maniac: he spent all his time in the lab or traveling. We all worked 14 or 15 hours a day. Everybody was so competitive, and we wanted to prove ourselves, so we would do anything," Tsai says. "I would not say that it was the most pleasant time. However, it would be hard to find any other place where you could learn so much and get so much done."
It was here that chance came into play. Tsai and a graduate student were the first to isolate a family of cyclin dependent kinases: little processing units on a cell's surface that take in signals from the environment, integrate those signals with others, and alter the functions of other intracellular proteins. (Kinases are enzymes, all of which act by causing chemical changes in proteins.) Although they set out to study cyclin dependent kinases in malignant cells, Tsai became intrigued with a member of this family of enzymes, called cdk5, which is peculiar to nerve cells.
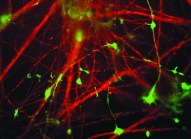 |
| An image from the laboratory of Li-Huei Tsai shows a protein, in green, associated with growing structures in cultured young cortical neurons. |
| Courtesy of Li-Huei Tsai |
Nothing else Tsai had studied was as interesting as this, "and when I get excited," she says, "I cannot stop myself." Harlow supported her desire to pursue research on cdk5 in the brain. But her friends thought she was crazy to leave cancer for neuroscience, because if she switched her focus so late in her postdoctoral training, who would hire her as a faculty member? The answer turned out to be Peter Howley, M.D. '72, now Fabyan professor of comparative pathology and chair of the HMS pathology department. Although this strong basic-science department emphasizes the fundamentals of biology, it is also a place where, as Joseph Martin says, researchers like Tsai "are turning their interests to work on problems that our patients are worried about."
During healthy brain development, the team of cdk5 and p35 do only good works. But Tsai and her colleagues found that when cdk5 is paired with p25, a truncated version of p35, it's bad news. Helpful p35 is chopped into dangerous p25 by an enzyme that rises rapidly in the brain following a stroke, or slowly and steadily in the presence of substances associated with the formation of the amyloid plaques in Alzheimer's disease. As levels of cdk5 and p25 rise, they alter the structure of an ordinarily harmless protein, tau, so that it becomes a building block for neurofibrillary tangles. These abnormal deposits, along with amyloid plaques, are hallmarks of AD.
Major pharmaceutical companies have eagerly followed reports from Tsai's lab, and several are already working on cdk5 inhibitors as potential AD treatments. Tsai's instinct, however, is that blocking this pathway alone won't be sufficient to stop AD. She believes that a cocktail of drugs will be required to halt neurodegeneration, just as combination therapies are required for AIDS and many cancers.
Tsai's group uses a top-of-the-line mass spectrometer to identify literally thousands of proteins that might be targets for treatment in patients with AD. This device enables researchers to detect cdk5-p25 induced abnormalities in hundreds of candidate proteins in a single day. Without this technology, Tsai marvels, "it would probably take another 20 years of work in multiple labs to reach the same conclusions."
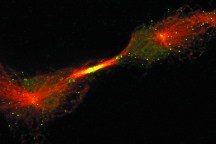 |
| One of the proteins Tsai studies, shown in green, concentrates at the midbody of dividing cells. |
| Courtesy of Li-Huei Tsai |
There is no doubt that Tsai's own dreams have carried her far. Over the past seven years, she has made discoveries that could benefit millions of people. And when she thinks of her much-loved grandmother, in that small fishing village outside Taipei, and of the possibility that her findings may someday enable physicians to effectively treat patients with Alzheimer's disease, she says, "I feel very proud of my research."
Cell Death: The Chemical Biology of Stroke and Brain Illnesses
Junying Yuan also had an influential Chinese grandmotherin her case the matriarch of an intellectual family battered by the Cultural Revolution: family members were forced to denounce one another, reputations and careers were lost, and homes and properties were destroyed or confiscated. Yuan's parents were professors at Shanghai Medical School, but when she was 10 her father, who had been under tremendous political pressure, died of sepsis following a botched surgery. Her mother's mental health and teaching career collapsed as a result. Yuan's indomitable grandmother kept the family together and emphasized, despite the grimness of the present, that there were no limits on what Junying could accomplish in her life.
Apparently grandmother was right, because today Yuan is a professor of cell biology at HMS and heads a thriving, 19-person laboratory working toward new therapies for stroke, Alzheimer's, and Huntington's disease. The common thread that connects these devastating conditions is a special kind of cell death, called apoptosis, which her discoveries catapulted into prominence. "Junying, by cloning the first two cell-death genes, made the major discovery that opened the whole field," says Berry professor of neurobiology Edward A. Kravitz, Yuan's first mentor at the medical school. She initially found two cell-death genes in a worm; in 1993, she identified the first one in human cells.
 |
| Appalled by the effects of Huntington's disease, Junying Yuan has probed the mechanisms of cell death, leading researchers to the epicenter of strokes. |
| Photograph by Tracy Powell |
Generations of pathologists had described characteristic patterns of cell loss in the brains of people with Parkinson's, Huntington's, or Alzheimer's disease. Yet doctors weren't particularly curious about why these cells died. "When Junying started on this, looking for cell death genes, it was way out in left field," Kravitz recalls. He was more sympathetic than most people, at least in part because Yuan's interest in neurodegeneration was sparked by "Neurobiology of Disease," a course Kravitz initiated (and still teaches) at HMS. His students, who are in Ph.D. programs, not medical school, read scientific articles about major brain diseases and attend classroom presentations by patients and their physicians to see firsthand how nervous-system disorders affect individuals and families. Kravitz hopes students will ask themselves, "How is science going to solve these diseases?"
The course worked its magic on Yuan. She was powerfully affected by a thin, relentlessly moving man with Huntington's, and was appalled to learn that modern medicine could do nothing for him. She suspected that a genetic program for cell death was involved in neurodegenerative diseases such as this, but no one except Kravitz seemed interested. Finally she located H. Robert Horwitz at the Massachusetts Institute of Technology. "He was the only one in the world working on this problem of cell death, trying to get to the bottom of it," she says. Although Horwitz was not officially part of a joint neuroscience program that HMS and MIT had recently created, Yuan was able to join his lab but still receive her doctorate from Harvard.
Staying at Harvard was important to her, because being invited to come was such an extraordinary opportunity. After the United States and China reestablished diplomatic relations, a group of American biochemists administered an annual examination to about 25,000 Chinese students, seeking to identify 50 or 60 who would be offered scholarships at U.S. graduate schools. Yuan, a biochemistry major at Fudan University in Shanghai, was the top scorer in 1982. She was recruited by Harvard, where she experienced considerable culture shock despite her enthusiasm for grad school. This was cushioned by the relative nearness of her future husband, who had been brought to the University of Rochester by the same program. Today he is a cancer researcher at Boston University and they have two children, 8 and 11, who are old enough to be described by their mother as "a lot of fun."
In the Horwitz lab, Yuan began studying genes that turn out to be key players in apoptosis, a genetically programmed process by which healthy cells commit suicide, rather than sliding slowly into senescence and death. Apoptosis is essential for normal development: human embryos have webbed fingers and toes, for example, until apoptosis causes the webs to fall away. Although that's a good thing, apoptosis in the adult brain is generally not.
The genes that Yuan has identified in the past 15 years encode caspases, enzymes that are versatile actors in the drama of cell death. In ischemic stroke, for example, cells die first in the area that is abruptly deprived of blood, and then caspases seep into surrounding tissue and kill more and more brain cells. Yuan discovered this by collaborating with professor of neurology Michael Moskowitz, who treats stroke patients at Massachusetts General Hospital. Working with a special strain of mice, they identified a drug that blocked certain types of caspase activity and thereby lessened stroke damage. What's more, the drug limited peripheral cell death even when it was given several days after the eventencouraging news because present-day stroke treatments are only beneficial if used within hours of the event.
After Moskowitz and Yuan published their results, several pharmaceutical companies began developing drugs to inhibit the specific caspases involved in stroke. Yuan is not involved in these efforts, because she thinks it will be difficult to develop an inhibitor that is safe enough for human use. Besides, she is now focused on what happens at ground zero, where the abrupt loss of blood supply causes cells to die of necrosisa type of death that does not involve caspase activity. Yuan's team hopes to learn how necrosis works, and in the process develop new ideas for treating stroke patients. The payoffs are obvious: "If you can prevent 70 percent of cells from dying in stroke, or maybe even 50 percent," Yuan says, "people would be able to lead a pretty normal life, instead of being incapacitated."
In order to learn more about necrotic cell death and possibly identify new drugs, Yuan's lab is collaborating with Harvard's Institute of Chemistry and Cell Biology (ICCB), a unique enterprise that marries cutting-edge chemistry with the latest in laboratory automation (more details are available at http://sbweb.med.harvard.edu/~iccb). The institute was the brainchild of FAS chemists, who have made thousands of molecules that might be medicines, and medical-school scientists, who put together a system that can evaluate as many as 1,500 of these compounds at once and spit out understandable results. These remarkable tools, once available only at major pharmaceutical companies, are now accessible to any Harvard researcher who needs them. Scientists who think they have identified a possible drug target, such as a gene or protein, use ICCB's library and equipment to test the efficacy of myriad potential drugs quickly, homing in on those that appear biologically active. ICCB technology enables researchers to screen as many as 16,000 candidate molecules in a week, winnowing that huge number down to 10 or fewer that look promising enough to merit more intense study.
The workhorse of this system is a 384-well plate that looks like a finely perforated white plastic waffle, where each perforation holds a discrete experiment. Yuan's necrosis experiments involve placing in each well a certain type of human cell, a chemicalobtained from huge libraries amassed by Harvard, the National Institutes of Health, and various commercial suppliersthat would ordinarily induce apoptotic cell death, and a caspase inhibitor that blocks apoptosis. This forces the cells to take the other fork in the road, which is necrosis. These conditions are held constant. The variables are introduced by a robot that adds precise quantities of 384 different compounds to the basic set-up, one to each well. The plates are fed into an automated plate reader that looks no more imposing than a photocopier. Working at mind-boggling speed, the reader checks the condition of cells in each tiny well and generates a display showing whether they are alive or dead. If they are alive, then whatever was added to the well blocked necrotic cell death.
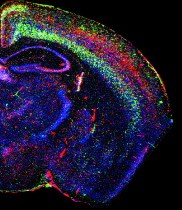 |
| Three different variants (red, blue, and green) of Class I MHC molecules in an adult mouse brain. New technology helps researchers trace the complexities of brain function far beyond the single-cell studies of the recent past. |
| Courtesy of Carla J. Shatz |
Using ICCB's high-throughput chemical screening, one team in Yuan's lab is looking for possible Alzheimer's treatments. These would act by blocking caspase 12, which is not involved in stroke damage but instead makes brain cells vulnerable to toxins released by amyloid plaques in AD patients. If no caspase 12 is present, amyloid doesn't have the same devastating effect on brain cells, so the team is seeking a safe and effective caspase 12 inhibitor. Another lab project can be traced back to the Huntington's patient whose plight first aroused Yuan's interest in the death of cells. It seems that caspase 8 is summoned by abnormal proteins in the brains of people with Huntington's, where it then kills the cells that called it. Yuan and her colleagues are seeking drugs that might keep this from happening, too.
There are no quick fixes for any of these problems, but technology such as the ICCB screening system is causing an explosion of knowledge about brain diseases. In the future, Yuan says with conviction, "Neurologic diseases are going to be much more treatable than they are now."
From Impulse to Motion: Huntington's and Parkinson's
When better treatments do become available, they will have been clinically tested at leading academic medical centers such as Massachusetts General Hospital, where in 1991 Anne Buckingham Young was appointed chief of neurology and Dorn professor of neurology at HMS. She was the first woman chief of service in the hospital's 180-year history, a record that Joseph Martinwho vacated the posts that she stepped intocalls "embarrassing." (Shortly after Young's appointment, Patricia K. Donahoe was named chief of pediatric surgery, a subspecialty at MGH's in-house Hospital for Children.) Today, Young leads a department with nearly 300 physicians, scientists, and staff, plus 36 young doctors in residency training. The neurology service has 60 regular hospital beds and a 17-bed neurology intensive care unit, and last year cared for 20,000 outpatients. Annual funding for research stands at $18 million.
At the helm is a woman whose lack of pretense makes her the antithesis of what one former neurology resident calls "the classic stuck-up chief of service at Mass General." Young's maverick streak surfaced in childhood, when her father nicknamed her Tiger Annie "because I always came out with my fists up." She grew up in a North Shore suburb of Chicago, where she was sent to prep school so that she wouldn't fall in with the "wrong crowd" and get into trouble. At Vassar in the late sixties, she found plenty to get into. "I spent a lot of time off campus dating plumbers and smoking dope and all those things," she admits. But behind this hipster façade was a budding scientist whose secret vice was biochemistry. "I loved being in the laboratory: starting with an idea, asking if I could make it work, and fiddling around with gels and pipettes. It was just right for me," Young says. Working off-campus in a hospital lab, she liked "running the machines and getting the results and seeing how efficient I could be." The idea of taking care of sick people scared her, however, so she imagined earning a Ph.D. and spending her life in the lab.
 |
| A "maverick," Anne Buckingham Young, who has pioneered research on Huntington's and Parkinson's diseases, proclaims that "neurology is fun." |
| Photograph by Tracy Powell |
In fact, she enrolled in an M.D.-Ph.D. program at Johns Hopkins and finished both degrees in just five years. While working in a professor's lab, Young helped identify several neurotransmitters that carry signals from the brain to the body's moving parts. Her Ph.D. research focused on the seat of volitional movement, the basal ganglia, where the brain turns desire for a chocolate truffle into the action of picking one up. Normal basal ganglion activity is disrupted in both Huntington's and Parkinson's diseases, but their manifestations are dramatically different: people with HD can't stop moving, while PD patients often "freeze" and can't start.
Young and her husband, John B. Penney, became fascinated by such patients during their residencies at the University of California-San Francisco in the late 1970s. When they joined the neurology faculty at the University of Michigan, they let it be known that movement disorders were their specialty. So many patients were referred to them that "after lots of trial and error, we got pretty good at it," Young recalls. She understates the case: she and Penney helped discover the gene for HD, and their research laid the groundwork for the first surgical treatment approved for PD.
The discovery of the Huntington's gene is one of the best-known and most colorful sagas in modern genetics. Young and Penney got involved in this quest in 1981, when they met psychologist Nancy Wexler in Ann Arbor. Wexler's mother had died of HD, giving her and her sister a 50-50 chance of inheriting the disorder, and in the late sixties the Wexlers established the Hereditary Disease Foundation to spearhead the search for the HD gene. Wexler was looking for doctors to accompany her to Venezuela's Lake Maracaiboan isolated area where foundation-sponsored researchers had found a huge family plagued for generations by HD. Young signed up to go, while Penney agreed to stay home to manage the care of their two small daughters. When the children got a bit older, Penney joined Young in the annual expedition that provides medical care and obtains specimens from hundreds of family members; they shared the experience until his sudden death from a heart attack in 1999. The specimens were turned over to a team of geneticists at Massachusetts General Hospital, MIT, and the University of Indiana, who used them to locate a genetic marker for Huntington's disease in 1983, and to find the HD gene itself in 1993.
Young's research group at MGH has used the gene to create mouse models for HD, which enables them to experiment with drugs that might block the insidious progression of symptoms. To come up with candidate compounds, they are creating a high-throughput screening facilitymuch like Harvard's ICCB set-upat MGH's Charlestown research campus. The lab has already identified several drugs that slow the disease's progression in mice, including agents already approved for other illnesses. It remains to be seen whether these will also work in people.
Young and Penney also made a major contribution to the treatment of Parkinson's disease. In 1986, they wrote an article postulating that certain basal ganglia cells would be overactive in PD patients, and that electrical stimulation of two specific brain regions might reduce symptoms by calming this activity. Deep brain stimulation, which uses implanted electrodes, was approved by the Food and Drug Administration in 1997. The procedure is performed at MGH and other hospitals as a last-ditch treatment for patients no longer benefiting from anti-Parkinsonian drugs.
In 2000, Young became only the second woman elected president of the 127-year-old American Neu- rological Association. What impresses physicians who train on the MGH neurology service, however, is how down-to-earth the woman with the intimidating curriculum vitae actually is. In teaching conferences where pompous senior faculty might parade their erudition, Young often asks basic, central questions that her residents would be embarrassed to ask. And they are grateful. They see their chief mainly at grand roundslectures on clinical or basic research topicsand in "morbidity and mortality" conferences where the quality of patient careincluding serious mistakes by residentsis reviewed in great detail. "If there is one thing that you learn from Anne, it's standards. She always made it clear if she thought there was a right thing to do, but she also made it clear that she understood that everyone has limitations," recalls Jonathan Rosand, a former chief resident who is now an MGH staff neurologist and an HMS instructor in neurology. "I felt that I had to be perfect," he adds, "but I didn't feel I had to be perfect for her to like me."
In January, nearly 60 of Young's former residents threw a surprise party in her honora roast where they regaled the group with in-jokes, embarrassing stories about her and about themselves, and testimonials to her influence on them. After the party, it seemed to Young that they had learned the main lessons she hoped to impart. When residents finish their training, she says, "I want them to go away with the idea that neurology is fun, that science and investigation into neurology is even more fun, and that they should follow their imaginations."
Anne Young, Carla Shatz, Junying Yuan, and Li-Huei Tsai are among the many Harvard researchersmale and femalewhose creativity and determination are yielding new insights into the brain and its diseases. At the College, more than 300 undergraduates have signed up, through their concentrations in biology, computer science, history and science, philosophy, and psychology, to focus on a new course of study connected with the University's mind/brain/behavior interfaculty initiativeevidence that there is an enormous cadre of young people who want to get their hands, at least metaphorically, on the human brain. For his part, President Lawrence H. Summers emphasized the University's role in biomedical research in his installation address and continues to do so, suggesting that the early twenty-first century may become a golden age of brain research at Harvard.
| The Archives for Women in Medicine Women came late to Harvard Medical School. It wasn't until 1949, a century after Elizabeth Blackwell became the first female medical-school graduate in the United States, that HMS conferred its first M.D. degrees on women. Women have contributed much to Harvard and to medicine since then, but documentation of their accomplishments is scant. Of the 900 collections of personal papers held by the Countway Library, only 18 were created by women. The Joint Committee on the Status of Women and the Countway Library want to establish the Archives for Women in Medicine, which would record the contributions of outstanding individuals and document the social phenomenon of women in medicine. The first step is funding an archivist who could start building collections immediately. There is a sense of urgency because early women graduates are retiring, and irreplaceable materials may be lost. The long-range goal is to build a substantial endowment that would expand collections and make the archive an active center for scholarship and education. For information about the project, visit the archives website (www.hms.harvard.edu/jcsw/womenarchives.htm) or contact professor of radiation oncology Nancy J. Tarbell, M.D., at the Office for Women's Careers (at 617-724-5229 or care of Massachusetts General Hospital, 55 Fruit Street, Bulfinch 360, Boston 02114). |
Medical writer Patricia Thomas is the author of Big Shot: Passion, Politics, and the Struggle for an AIDS Vaccine.