Doctors once kept jars full of sugar pills, in various colors, in their offices. “Take two of these and call me in the morning,” they’d tell their difficult patients. In the 1950s, when the randomized controlled trial was developed as a procedure, scientists learned the sugar pills could indeed have an effect—termed placebo, Latin for “I shall please.” The studies turned scientists’ view of those pills on its head, just when the medical community began questioning the ethics of administering them. “They said it had huge effectsbut you’re not allowed to give it,” says assistant professor of medicine Ted J. Kaptchuk of the Medical School’s Osher Institute, which evaluates so-called holistic or alternative medicine and seeks to integrate it with Western medicine (see “The New Ancient Trend in Medicine,” March-April 2002, page 46).
The placebo effect has become so well-established that regulatory agencies now approve a new drug only after studies show that its effect exceeds that of a placebo. Still, much remains to be learned about the constellation of circumstances—expectations, perception, the power of positive thinking—that seemingly come together to create the effect. Kaptchuk, who studied and practiced Chinese medicine before coming to Harvard, has devoted his career to investigating the subject. In a recent study, he found that placebo acupuncture confers a more powerful effect than does a traditional sugar (or, in this case, cornstarch) pill.
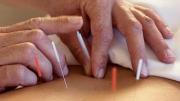
Kaptchuk studied 270 adults who reported moderate to severe pain, lasting at least three months, in one arm, and who rated their pain at least a 3 on a 10-point scale. He divided subjects into four groups: one received an analgesic in pill form; another, pills with no active ingredient; a third group received real acupuncture; and the fourth, fake acupuncture. (Kaptchuk falsified acupuncture by using specially developed needles that look just like real acupuncture needles—tiny swords with a copper-coil handle—but whose shafts retract into the copper coils when pressed against the skin. The patient feels a pin prick, but there’s no actual penetration. Even Kaptchuk was fooled: “The first time someone gave me a dummy needle, I said, ‘You made a mistake. You gave me the real needle.’”)
The pill-takers spent eight weeks in treatment, the acupuncture patients six, and all had two appointments a week. (The researchers determined the minimum effective time frame for each treatment and, as a recruitment incentive, offered to treat subjects from each placebo group with the actual therapies once the study ended.) The results, published in the British Medical Journal, found that the “improvement slope” of the line that plotted the decrease in pain was more than twice as steep for the subjects who received placebo acupuncture as it was for those who took placebo pills. The sham acupuncture recipients also scored significantly better than the cornstarch pill takers on the Levine symptom severity scale, which factors in the severity, frequency, and duration of symptoms such as pain, numbness, and weakness. (Kaptchuk declined to say which treatment—real acupuncture or real analgesic—was more effective; that comparison will appear in a forthcoming study.)
For now, Kaptchuk isn’t sure why sham acupuncture seems effective at relieving patients’ symptoms. It could be the time invested, or the human contact—the patients in the pill groups received only follow-up phone calls, rather than in-person appointments. But Kaptchuk believes there was something about the act of placing needles on the body, whether those needles pierced the skin or not: “All medicine is a ritual,” he says.
Further evidence for the placebo effect appeared in the incidence of side effects among subjects who received such treatments (see “The Nocebo Effect,” May-June 2005, page 13). Nearly a fifth of the patients who underwent sham acupuncture reported pain during treatment, while nearly a quarter of the placebo-pill takers reported dry mouth; even more reported feeling drowsy. “We had people on the placebo pill…saying they were so tired they couldn’t function,” Kaptchuk says. (The solution: cutting the dummy pill in half to provide a smaller “dose.”) The side effects reported by the placebo-group subjects exactly mirrored the side effects described by the researchers at the study’s onset. That finding “gives us very good evidence that how you tell patients to monitor possible feelings actually precipitates those feelings,” Kaptchuk said. It also has direct clinical implications for how doctors and drug companies should describe treatments’ side effects. Ironically, Kaptchuk adds, the placebo effect doesn’t exist even as a concept in Chinese thought, where an effect is an effect, placebo or not.
~Elizabeth Gudrais
Osher Institute website: www.osher.hms.harvard.edu