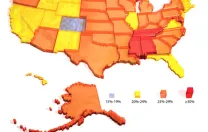
Plain and simple, humans are becoming more obese and more diabetic. Although genetic factors undoubtedly contribute, the pace of change is so fast that the explanation cannot possibly lie in changes in our DNA.
But the recognition that environmental factors are vitally important to the obesity and diabetes epidemic is roughly where the consensus ends. Most scientists working in the area agree that some variation of too much food and too little activity is to blame. But others say the real problem is the wrong type of food—and even here there is disagreement about whether the chief culprit is too much sugar, too many carbohydrates in general, too many refined (as opposed to complex) carbohydrates, too little fiber, or too much animal fat.
And food and exercise are not the only environmental factors that matter. Some experiments have shown that sleep deprivation causes hormonal changes that ramp up hunger; a study published this year found that poor sleep quality impairs the body’s ability to regulate blood sugar. One recent paper linked increased diabetes risk to chronic, low levels of arsenic in drinking water; another linked obesity to high levels of monosodium glutamate (MSG) consumption. But teasing out the relative importance of each influence is, in some sense, an academic exercise.
Diet and exercise are still the most powerful ways to protect against diabetes (see “The Way We Eat Now,” May-June 2004, page 50, and “The Deadliest Sin,” March-April 2004, page 36). But getting people to follow this advice is difficult—particularly when the cheapest and most convenient foods are often the least healthful, and government policies contribute to the problem by subsidizing the production of high-fructose corn syrup and livestock feed, making fresh produce relatively more expensive.
Professor of genetics and of medicine David M. Altshuler cites an experiment that reduced the progression to diabetes by two-thirds in a prediabetic population. That study provided people with exercise coaches and dietitians—the kind of one-on-one attention and monitoring that keep celebrities lean and fit, but are expensive and, says Altshuler, “unrealistic to apply in a broad-based way across the country.” Even with that intensive intervention, he notes, some of the subjects still developed diabetes. “The rate in the control group was 10 percent per year,” he says. “Slowing that by two-thirds was really great—but people were still getting diabetes.” Other than bariatric surgery (which reduces the size of the stomach), says Altshuler, “the available treatments are just not very effective.”
Even as scientists acknowledge the importance of behavior, they recognize that we are human and prone to falling off the wagon. A diet that succeeds fabulously in mice may be impossible to replicate in people, short of locking subjects in a lab and physically preventing them from eating more than a certain amount.
The notion of thinness as a badge of superior will power rankles some researchers. “Even today, at least 30 percent of people maintain normal body weight without thinking about it very much,” says associate professor of medicine Eleftheria Maratos-Flier, an endocrinologist who treats obese patients at the Harvard-affiliated Beth Israel Deaconess Medical Center and researches the hormonal signals and neural pathways that regulate energy balance. Although many people stay lean only through vigilant eating and exercise, others can eat vast amounts of food day after day without becoming obese. Some studies have found people who fail to lose weight despite very low caloric intake. Learning more about genetic variation can help explain why some people stay thin without trying. This, in turn, points to therapies that may help bridge the physiological gap between those who are prone to obesity and those who are not.
The study of individual variation also points to lifestyle-change strategies that don’t set people up for failure. Research by associate professor of pediatrics David S. Ludwig, who directs the Optimal Weight for Life program (www.optimalweightforlife.com) at the Harvard-affiliated Children’s Hospital Boston, has revealed an apparent biological explanation for individuals’ varied responses to the same weight-loss regimen. Ludwig has found that the population falls into two groups—rapid insulin secreters and slow insulin secreters. When given an oral glucose solution, the ultimate simple carbohydrate and the common test for diabetes, people in the first group show a pronounced spike in insulin secretion; such spikes can lead in turn to low blood sugar and hunger. The latter group, with more gradual insulin release, avoids this roller-coaster effect.
In an 18-month randomized controlled trial of obese young adults, slow insulin secreters lost the same amount of weight on a low-fat diet as on a low-glycemic-load diet (rich in fat, protein, and slow-digesting carbohydrates such as vegetables and whole grains). The rapid insulin secreters, in contrast, lost five times more weight on the low-glycemic diet than on the low-fat diet. Probing individuals’ distinct biology this way can help explain why some dieters find the pounds melting off, while others find weight loss stubbornly elusive, says Ludwig: “The individuals who do well on a low-carb diet may not be the same individuals who do well on a low-fat diet.”
Take another example: eating seafood regularly and consuming one alcoholic drink per day are generally considered ingredients of a healthy diet. But professor of nutrition and epidemiology Frank B. Hu has found that for people with a condition called hyperuricemia—excess uric acid in the blood, a condition genetic in origin and more common among Asians than in the general population—these same dietary choices further heighten uric acid levels and, consequently, diabetes risk. Hu and others have also published findings of increased diabetes risk for people with an elevated level of iron in the blood: for certain people whose bodies are genetically primed to absorb iron with particular efficiency, iron supplements may harm, not help.
Such knowledge may one day produce personalized prescriptions for losing weight and avoiding diabetes. For now, they point to one conclusion, says Walker professor of medicine Jeffrey S. Flier, an obesity researcher who is dean of Harvard Medical School (and Maratos-Flier’s husband): “It isn’t as simple as eating less and exercising more.”