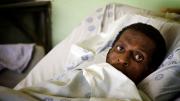
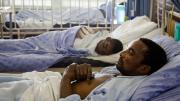
Sitting around a table at Edendale Hospital, in Pietermaritzburg, South Africa, the traditional healers tell their story. It used to be that they could heal people. Then, slowly, there were more and more cases where their medicines didn’t work.
The symptoms followed a pattern, and they looked like something the healers knew well: ancestral problems, unresolved conflicts with deceased relatives. But the rituals to resolve these ancestral issues—the remedies passed down through generations of traditional healers—didn’t work. The healers realized they were dealing with a new disease, one no amount of making peace with one’s forebears would cure.
Across Africa, two healthcare systems exist largely in parallel: the medical establishment scorns traditional medicine, and traditional healers are excluded from the framework of hospitals, clinics, and pharmacies. But one innovation-minded program aims to improve care for people with HIV and tuberculosis by bridging this gap: by training traditional healers and inviting them into the system.
Four-fifths of South Africans consult a traditional healer before heading to a doctor, notes Krista Dong, the Harvard Medical School lecturer and Massachusetts General Hospital (MGH) infectious-disease physician who directs the iTEACH program. (The program, whose name stands for Integration of TB in Education and Care for HIV/AIDS, is an initiative of the Ragon Institute of MGH, MIT, and Harvard, with primary funding from Richard Witten, J.D. ’78, and his wife, Lisa; and additional funds from Daniel and Marjorie Sullivan.)
iTEACH is acutely aware of the trust black South Africans place in traditional healers, and treats this trust as a resource. Sixty healers have completed iTEACH’s three-day prep course and the government-approved course for HIV counseling; iTEACH successfully lobbied for that course to be offered in Zulu. (It was previously taught only in English, which almost none of the traditional healers speak.) Those who demonstrate exceptional commitment and leadership continue on to a clinical internship with iTEACH at Edendale, the government hospital where the program is based. The interns assist with HIV care in the medical wards and conduct training for patients who are starting antiretroviral therapy (ART), to learn more about the care their clients will be receiving in the Western system. Traditional healers who have completed this training include both sangomas, who are called by their ancestors to the role, and inyangas, herbalists who choose the profession. The healers work alongside iTEACH staff in HIV testing drives, and are being trained to conduct testing drives and educational sessions in their communities. The healers also receive training in identifying symptoms of HIV infection, tuberculosis, and drug side effects, and upon completing the iTEACH course are qualified to refer patients directly to a clinic, thus officially integrating them into the system.
Almost all physicians in South Africa discourage the use of traditional medicine, says Dong. But even though some traditional potions do interfere with HIV medication or exacerbate symptoms, Dong believes the doctors’ intolerance “only serves to alienate patients.” She says the majority of patients are receiving “dual care” from a clinic and a traditional healer and “will continue to do so despite what a doctor says.” Instead of trying to persuade patients not to consult traditional healers, Dong believes doctors should accept that patients are going to be using traditional remedies and negotiate with the patient about how to do so more safely.
Demonstrating respect for traditional medicine is a hallmark of iTEACH’s approach. For example, the traditional practice of twasa, or induced vomiting, can further weaken a patient with acute TB infection or one who is just beginning ART. Those patients are often feverish and dehydrated; the iTEACH recommendation, given both to healers and to doctors with whom the organization works, is not to prohibit twasa but to delay it until the patient's prescriptions have a chance to work. (When patients do begin twasa, the healers give precise instructions about when to purge so the practice doesn’t interfere with ART; Dong notes that similar instructions are given to mothers of infants with HIV, given babies’ propensity for spitting up their food.)
The healers do not discount the power of Western medicine. “The ones we work with all accept that traditional medications do not cure HIV or TB,” says Dong. Rather, they recognize that herbal remedies “can be used as adjunct treatment, in close communication with the clinic doctor.” In an effort to foster mutual respect and raise awareness, iTEACH regularly takes groups of doctors to visit traditional healers and learn about their work.
iTEACH holds Western and traditional medicine equal, says Dong: acknowledging, for example, that ART drugs also have side effects. With this approach, says Dong, "The healers don't feel threatened, as we don't discourage patients from engaging in traditional practices."
Connecting the healers into the healthcare system has another advantage: it reaches patients who would never make it to a doctor’s office. Traditional healers outnumber physicians by nearly 10 to 1, so potentially, well-trained healers can bring sound medical care to large unserved swaths of the population. “Having traditional healers involved in the epidemic, able to recognize things that need treatment that we can provide at the hospital or through medications, is really key,” says professor of medicine Bruce Walker, Dong's mentor and the founder-director of an HIV immunology research lab in nearby Durban.
The project with the traditional healers is just one component of iTEACH. Although the Ragon Institute’s focus is HIV immunology and vaccine research, iTEACH seeks to support treatment for infected patients. It has helped decentralize ART, bringing it to rural clinics so patients don’t have to travel so far for their prescriptions. Beyond this core work, iTEACH searches for innovative ways to increase access to care and to improve treatment adherence. Integrating TB diagnosis and treatment is crucial: the disease is the number-one killer of HIV patients, whose weakened immune systems are especially susceptible.
Multifaceted and flexible, iTEACH above all seeks to be open to creative ideas, with an eye for what can be efficiently and cheaply replicated in multiple locations and at large scales. The program convinced mobile-phone service provider MTN to donate advertising space on text messages to promote a call-in HIV information line iTEACH operates, resulting in a threefold increase in call volume. A collaboration with a popular South African hip-hop artist led to the development of an HIV self-test that would be widely available free of charge. National law requires that counseling accompany HIV testing; the self-test, still in development, would include a toll-free number to contact a counselor, and iTEACH hopes the government will consider this as satisfying the requirement and allow distribution of the test.
This is not the only time iTEACH has pushed the political envelope: Dong and iTEACH deputy director Zinhle Thabethe joined thousands of activists in protests of the South African government's delay in providing ART. Last year, during a hiring freeze on staff positions in government hospitals, the pharmacists at Edendale found themselves working late into the evening to serve the many patients waiting for their medicines. The hospital’s decision to start a waiting list for ART—and thus stem the increase in the number of patients, and keep the pharmacists’ work day from growing longer—attracted media attention. Although Dong says the decision was just an effort to avoid overworking the pharmacists, it wasn't long before the government authorized Edendale to hire more pharmacists.
South Africa is one of Africa’s most prosperous countries, but that has not helped it escape the HIV crisis. Infection rates 20 years ago were much lower here than in west, central, and eastern Africa, but have skyrocketed as some other countries have brought their epidemics under control. Today, South Africa’s infection rate is the fifth highest in the world, and KwaZulu-Natal province, on the country’s eastern coast (where Durban and Pietermaritzburg are located), is the epicenter.
Nor does South Africa’s relative prosperity mean government hospitals are equipped to handle the epidemic. Edendale, where iTEACH is based, has 900 beds, including 200 intensive-care berths—but only two ventilators. There are no heart monitors. When a patient goes into cardiac arrest, there is usually little the staff can do. The nurses are supposed to wear face masks, but the hospital is out of stock. Edendale lacks the measures universally in place in facilities in wealthy countries for treating illnesses as contagious as tuberculosis: rooms with negative air pressure, antimicrobial lighting, even isolation. “The whole city,” says Dong, “would be quarantined if this were Boston.”
Across southern Africa, the population’s genetic makeup and the specific strains of the virus that infect people there have interacted to produce higher transmission rates than anywhere else in the world. This was part of what drew Bruce Walker to establish a research site there in 1998. But when he arrived, he remembers, “I was unprepared for the enormity of the epidemic. It was just staggering. HIV permeated all aspects of daily experience. There were so many people infected, so many people affected.”
Besides ravaging the general population, HIV is taking a toll on healthcare workers: 2,000 nurses die of AIDS every year (not because they were infected through their work, but because the infection rate in the general population is so high). With nurses and other health workers dying faster than new ones can be trained, if nothing changes, says Walker, “The whole fabric of society is just going to collapse.”
He came to believe he couldn’t conduct research without also doing something about the dire need for treatment. With funding from donors Mark Schwartz ’76, M.B.A. ’78, M.P.P. ’79, and his wife, Lisa, Walker’s team began offering ART to patients who took part in research studies before the drugs were generally available. Thus iTEACH was born.
Since then, iTEACH has grown to a full-time staff of 18. A major theme in the research by Walker’s team is the ruinous interaction between HIV and tuberculosis, which preys on weakened immune systems. Edendale is a recruitment site for this research—and yet, “curiously,” says Dong, “until this year, Edendale has never had a death from tuberculosis.” Short on staff and short on money, the hospital was declining to test patients for TB. But accurate recordkeeping is critical for all sorts of purposes—for international aid, for research like Walker’s, for persuading the national government to acknowledge the impact of TB. Thanks to iTEACH's input, the hospital now performs a culture on every patient who coughs. On average, 40 percent of those tests come back positive.
To improve care for TB patients at Edendale, iTEACH also arranged for a single worker to conduct patient intake, perform the test, carry the sample to the lab, receive the results, and notify the patient and the supervising physician. This work was previously distributed among as many as seven people, so patients weren’t getting their results and therefore weren’t being treated; Dong says the reason was often as simple as an illegible phone number on the patient’s intake form. A worker who won’t have to call the number later “doesn’t have a reason to care” whether or not it’s legibly written, she says.
HIV care, TB care, health-systems reform, behavioral economics, political advocacy—iTEACH’s efforts span them all. It’s this kind of interdisciplinary, multi-pronged approach that holds the most promise for making a dent in the HIV crisis, says Walker. He himself serves as a sort of “superconnector” in and around Durban: for people from Harvard’s sphere and beyond, researchers and clinicians, foreigners and locals. He has supported training of African scientists; youth education through soccer; and studies by young researchers on, respectively, fertility choices of HIV-positive adults and how a hospital’s layout affects patients’ treatment adherence. In a new interdisciplinary project, Walker’s team will study the immune response during the early stages of HIV infection in young women; in the same cohort, other Harvard scholars will examine the behavioral predictors of infection. Such holistic team efforts lead to greater understanding than narrowly focused studies of behavior or biology or health systems issues. This exemplifies the approach of iTEACH, and of Walker: “It’s all interlinked.”