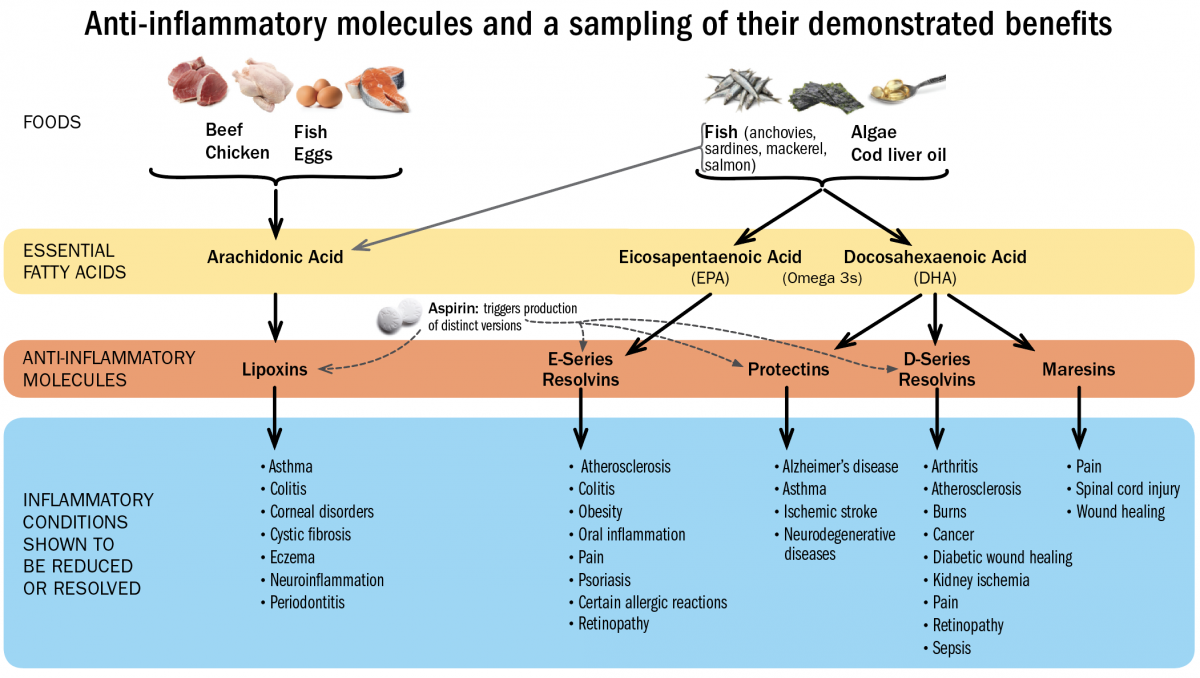
Of all the human immune system’s extraordinary capabilities, its capacity to regenerate and restore normal physiological function after an injury or infection is probably the least well understood. The process that resolves inflammation is separate from the familiar immune responses characterized by fever, redness, and swelling. Resolution of inflammation is controlled by a group of molecules called specialized pro-resolving mediators, or SPMs. These are distinct from other immune-system signaling molecules not only in their composition—they are lipids (fat-based) rather than proteins—but in their action: familiar immune cells destroy or engulf invaders and damaged cells, but pro-resolving mediators speed the healing process and can even prevent inflammatory diseases from taking hold in the first place.
At a Harvard Medical School conference on February 28—one of the last large symposia held there before COVID-19 put an end to such in-person gatherings—researchers shared their findings across a range of pathologies, from lung inflammation and wound healing to gingivitis and cardiovascular disease. The goal of this work, as Gelman professor of anaesthesia Charles Serhan explained in his introductory remarks, is to understand the physiology of resolution, in order to develop a pharmacology of resolution.
Serhan, who directs the Center for Experimental Therapeutics and Reperfusion Injury at Brigham and Women’s Hospital, presented an overview of the field. A little bit is known already about how to stimulate the body’s inborn processes of resolution, he said. Some statins mediate the production of certain classes of resolving molecules, and simple aspirin (in doses ranging from a nanogram to a picogram—a billionth to a trillionth of a gram) stimulates the production of other SPMs. A little is also known about how to avoid inhibiting the actions of SPMs that are naturally produced in the body. Many existing pharmaceuticals now used to treat inflammation, including NSAIDs such as ibuprofen, he explained, are actually toxic to the body’s innate ability to clear up inflammation on its own. So are steroids (which are broadly immunosuppressive and impair wound healing), COX-2 inhibitors (a subset of NSAIDs that can raise the risk of heart attack and blood clots), and biologics (engineered proteins that can dampen the immune response).
The hope is that SPMs, which exhibit none of the deleterious effects of existing anti-inflammatory therapies, might be developed into treatments for injuries, infections, and chronic inflammatory diseases (see “Raw and Red Hot,” a feature article about the role inflammation plays in myriad diseases). In animal models, SPMs have proven to be safe and effective therapies for a range of inflammatory conditions—in many cases, illnesses and tissue damage that are caused by an inappropriate or exaggerated immune response, such as arthritis, asthma, and atherosclerosis . They have also proven effective in speeding the healing of physical injuries. (An extreme example in animals is tissue regeneration in planaria, a flatworm, which is mediated by maresins, one of the four major classes of SPMs—the others are the lipoxins, resolvins, and protectins). Serhan asks: “Can we do this in humans?”
In humans, resolving molecules have been discovered at bioactive levels in fluids and tissues throughout the body: in tears, breast milk, urine, serum, plasma, synovial fluid in the joints, cerebrospinal fluid, and in the brain, lymph nodes, fatty tissues, the spleen, and the placenta. Synthesis of these beneficial molecules declines with age, and women may produce more of some of them than men. (In a study of the role of inflammation in gender differences in cardiovascular disease, when killed bacteria were injected under the skin of healthy human volunteers, raising a blister, women produced more resolvins and cleared the blister faster than men.) Research has also shown that patients with atherosclerosis, asthma, dry eye, arthritis, Alzheimer’s disease, and gum disease exhibit low levels of resolving molecules. Lower levels of SPMs are also found in obese patients and in smokers.
Presentations followed on resolution of inflammation in cancer and cardiovascular medicine, gum disease, wound healing, lung inflammation, and on the role of SPMs in the innate immune system generally. Professor of oral medicine, infection, and immunity Thomas Van Dyke discussed his research using SPMs to treat periodontal disease. Gum disease is an inflammatory condition in which bacteria raise an immune response that destroys gum tissue. Unchecked, the gums detach, and bone loss ensues. Anti-inflammatory drugs such as ibuprofen, steroids, and statins all attenuate disease progression, Van Dyke said, but none stop it entirely, and none reverse the effects of the disease. “We don’t use anti-inflammatories to treat it,” he said, “because they are toxic to resolution.”
In experiments with rabbits, however, topical treatment with resolving molecules prevented gum disease from ever occurring. Van Dyke has even shown that SPM therapy can reverse the disease, bringing the teeth and gums back to baseline.
In a phase 1 clinical trial involving human gingivitis—the first stage of periodontal disease—the treatment was found safe (demonstration of safety is the goal of phase-1 clinical trials).
The treated group did better than the placebo group, Van Dyke reported, and the results were also better than the best existing treatment, an antibiotic. Local application of the rinse also displayed a systemic effect, increasing pro-resolution molecules in serum. Van Dyke speculated that this might dampen systemic inflammation and slow the progression of inflammatory diseases beyond periodontitis.
Francis professor of medicine Bruce Levy, who is chief of pulmonary and critical care medicine at Brigham and Women’s, and had just been trained in suiting up for treatment of potential COVID-19 patients, spoke next, on the subject of lung inflammation. He presented evidence that six separate SPMs are actively bronchoprotective, anti-inflammatory, and pro-resolving, and showed that one SPM can increase the levels of another, to accelerate the healing process. In severe asthma, his research shows, SPMs promote the resolution of edema, the overaccumulation of white blood cells, the buildup of mucus, and airway hyperresponsiveness, all hallmarks of severe asthma.
Levy also showed a correlation between levels of SPMs and a variety of other lung diseases. A resolving molecule abundant in healthy human lung tissue is severely depleted in bronchitis, chronic obstructive pulmonary disease, and other ailments. Whether patients deficient in SPMs are more vulnerable to developing such illnesses is now a subject of active research interest.
Asked whether COVID-19 patients who develop the most severe and life-threatening form of the disease might similarly have a pre-existing deficiency in SPMs, Levy said that while there’s no direct evidence for this, anecdotally, he and some of his colleagues suspect so. The ability to synthesize SPMs declines naturally with age, a pattern consistent with the most severe cases of COVID-19, which disproportionately affect older patients. In fatal cases, victims appear to stage a massive immune response called a cytokine storm. Given that the patient’s response itself may be the proximate cause of these coronavirus deaths, a variety of drugs that target the inflammatory reaction are currently being tested for efficacy—not against the virus, but to see if they can dampen this damaging and sometimes fatal immune response. Furthest along in clinical trials (currently phase 3) is Actemra (tocilizumab), an inhibitor of the IL-6 inflammatory pathway that is approved for use in treating rheumatoid arthritis. The U.S. Biomedical Advanced Research and Development Authority is currently supporting accelerated evaluation of the drug’s effectiveness in COVID-19, and the FDA has given the go-ahead for tests of its effectiveness. Roche, the drug’s manufacturer, has reportedly already begun ramping up production, even without data proving its effectiveness.
Interestingly, prior research on SPMs has shown that some of them target the same IL-6 pathway, reducing inflammation in cases of both bacterial and viral infection. Serhan wrote in an email that he and Levy “suggest that resolvins and protectins could be helpful in reducing the cytokine storm and lung damage in COVID-19.” They are currently working with one of the symposium’s sponsoring companies to raise support for a small clinical trial of resolvin E1 in COVID-19 patients.
“We would be very lucky if this happens,” Serhan wrote, because it would highlight the role of therapies that support the patient’s own mechanisms for regenerating and restoring normal physiological function.