“Global health” typically brings to mind issues such as vaccination, maternal care, sanitation, and malaria control. It’s not usually associated with surgery. But consider the woman who dies in childbirth because she can’t reach a clinic that performs cesarean sections, or the man out of work because he can’t afford cataract surgery to restore his vision, or the child whose life is cut short by an injury that local healthcare workers don’t have the training to repair.
A landmark report published by the Lancet Commission on Global Surgery argues that a lack of access to safe surgical care has a major impact on the health and well-being of people around the world. A public conference at Harvard Medical School (HMS) on May 6 marked the report’s launch, following a similar meeting in London. “We want surgery to be part of the discourse on global health, and we want surgery integrated into the discussions about how you build health systems,” says John Meara, Kletjian professor of global surgery at HMS, one of three commission co-chairs.
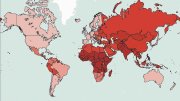
The problem is vast. “Five billion people cannot access safe, affordable surgery,” Meara said during his opening address in Boston. That number includes people who can’t afford expensive procedures as well as those who live far from an operating room. Closing the gap would require 143 million additional procedures each year. But the commission laid out an ambitious plan to achieve 80 percent coverage of essential surgical and anesthesia service per country by 2030, and outlined specific recommendations, goals, and indicators of progress that can be used to realize it.
The Lancet, a preeminent medical journal based in London, formed the commission in 2013 when a small group of surgeons joined with Justine Davies, editor-in-chief of Lancet Diabetes & Endocrinology, to champion an in-depth look at surgery around the world. The commissioners worked with collaborators from more than 110 countries to produce the report, focusing on surgery and anesthesia in low- and middle-income countries. Meara, who became the inaugural Kletjian professor this April, has been a leading advocate for putting surgery on the international agenda; his newly endowed chair is among the first global surgery professorships established at an academic institution.
Surgery has a role across the entire spectrum of human disease, and conditions that can be surgically treated represent about 30 percent of the global burden of illness. But high out-of-pocket surgical costs push 33 million people into financial catastrophe each year (and 48 million more when indirect costs like transportation are included). Achieving the commission’s 2030 goals would require a $420-billion investment. This staggering cost could yield major returns, though: the report projects that the lack of surgery and anesthesia would cost low- and middle-income countries $12.3 trillion in that span, a 2 percent drag on growth each year. During a talk at the conference, Gavin Yamey, a biostatistician at the University of California San Francisco School of Medicine, said,“Many surgeries are equally [as] cost-effective as other public-health measures.”
“To achieve our vision, we need people on the ground,” said commission co-chair Lars Hagander of the World Health Organization [Corrected June 17, 2015: he is affiliated with Lund University in Sweden] in a talk on workforce education: not only surgeons, but anesthesiologists, nurses, radiologists, pathologists, technicians, and rehabilitation specialists. That means providing medical training, as well as incentives for health professionals to stay in their local communities rather than move to high-income areas. In some cases, it may also require shifting some surgical duties to people with less training.
Equipment, supplies, and facilities are also needed. Yet a panel discussion on the role of industry in global surgery pointed out that in resource-poor areas, well-meaning donations can overwhelm clinics and nongovernmental organizations with old, faulty equipment and useless items they then must struggle to dispose of. “Equipment donation alone is not going to fix the problem,” said Asha Varghese, director of global health programs at the GE Foundation; it’s also necessary to train technicians who can operate and repair equipment to keep it running.
Another problem is data collection. “We have no idea how much the world is spending on surgery,” said Meara in his address. (The commission found that only two countries, Georgia and Kyrgyzstan, track those totals.) He and his fellow commissioners identified three “bellwether procedures” that can be used to assess the basic surgical-capability level of a nation’s healthcare facilities: cesarean section, abdominal surgery, and orthopedic surgery for bone fractures. Facilities that can handle those three interventions can easily manage a wide range of procedures.
Historically, global surgery has been most identified with medical missions—teams of surgeons who travel to resource-poor areas to perform procedures like cleft lip and palate repair or cataract surgery, which local people can’t otherwise afford. Such intermittent missions have saved lives and improved the health of many patients, but they have also been critiqued for not offering a lasting solution to the larger problems of healthcare delivery in those areas. As a result, the field has increasingly focused on building local capabilities.
Many talks at the conference focused on the respective roles of students, residents, surgeons, and academic researchers from high-income countries in improving surgical care internationally. Speakers said that young medical students and surgeons want to get involved in global health but need more opportunities to do so. HMS, for example, offers a one- to two-year global surgery fellowship that enables surgeons to provide surgical care or conduct research in low-income countries, and a one-year research associate position that allows medical students to participate in existing faculty-led programs abroad. Similar fellowships, and exchange programs that let surgeons spend extended time in needy areas, are becoming more common at medical schools and hospitals generally. The American College of Surgeons in 2004 launched Operation Giving Back to help connect surgeons to volunteer opportunities around the world.
But speakers cautioned that programs to improve care in other countries must respond to local needs. “We need to get away from surgical colonialism,” said Ainhoa Costas-Chavarri, a hand surgeon at Boston Children’s Hospital. Instead, many participants used the word “accompaniment,” an approach advocated by Paul Farmer, co-founder of Partners In Health. Robert Riviello, director of global-surgery programs at the Center for Surgery and Public Health at Brigham and Women’s Hospital, discussed one example, launched in 2012: a seven-year partnership between several U.S. academic medical centers and the Ministry of Health in Rwanda, that aims to boost training for healthcare workers in that country and transfer all clinical and teaching duties to local Rwandans by the program’s end. It’s important, Riviello said, not to arrive in another country with a set curriculum, but to plan together instead: “We shouldn’t assume we want the same things until we actually talk about them.”
In a keynote address, Farmer, now Kolokotrones University Professor of global health and social medicine, said that fixing the “grotesque disparities” in surgical capabilities requires strengthening health systems as a whole. “Building local capacity is critical to the advancement of this agenda,” he said. He also cautioned that a culture of safety in high-income countries should not become an excuse to avoid engaging with and practicing medicine in low-income countries. “It is not safe to perform surgery in most of the places we’re talking about,” he said, and yet there is ample need for surgical treatment, so turning away because of safety concerns is not a solution.
The Lancet report also included success stories about partnerships that have improved surgical care in Haiti, Mongolia, Uganda, and elsewhere. The commission is now working with the Republic of Zambia to begin assessing that nation’s surgical capabilities, based on the approach outlined in the report. Commissioners have also met with several other nations’ ministers of health and finance to make the case for investing in surgery. Meara emphasized that the real work is just beginning. “We’re not celebrating the completion of the project,” he said at the end of the meeting. “We’ve got a long way to go.”